Menopause is a natural phase in a woman’s life, yet for many, it brings a frustrating and often unexpected change: weight gain. This article explores what menopause is, why it is linked to weight changes, and how the right combination of medical support, diet and exercise can help give you a better understanding of the menopause.
What is Menopause?
Menopause marks the end of menstrual cycles. It is diagnosed after 12 consecutive months without a period and typically happens between the ages of 45 and 55, with the average in the UK around age 51.
However, symptoms can begin much earlier in a phase known as perimenopause, which often starts in the mid-40s. Some women experience early menopause, known as premature ovarian insufficiency, before the age of 40.
During menopause, the ovaries reduce production of key hormones including oestrogen, progesterone and testosterone. These changes affect much more than reproductive health. They influence everything from mood and memory to weight, sleep and energy.
What are the Symptoms of Menopause?
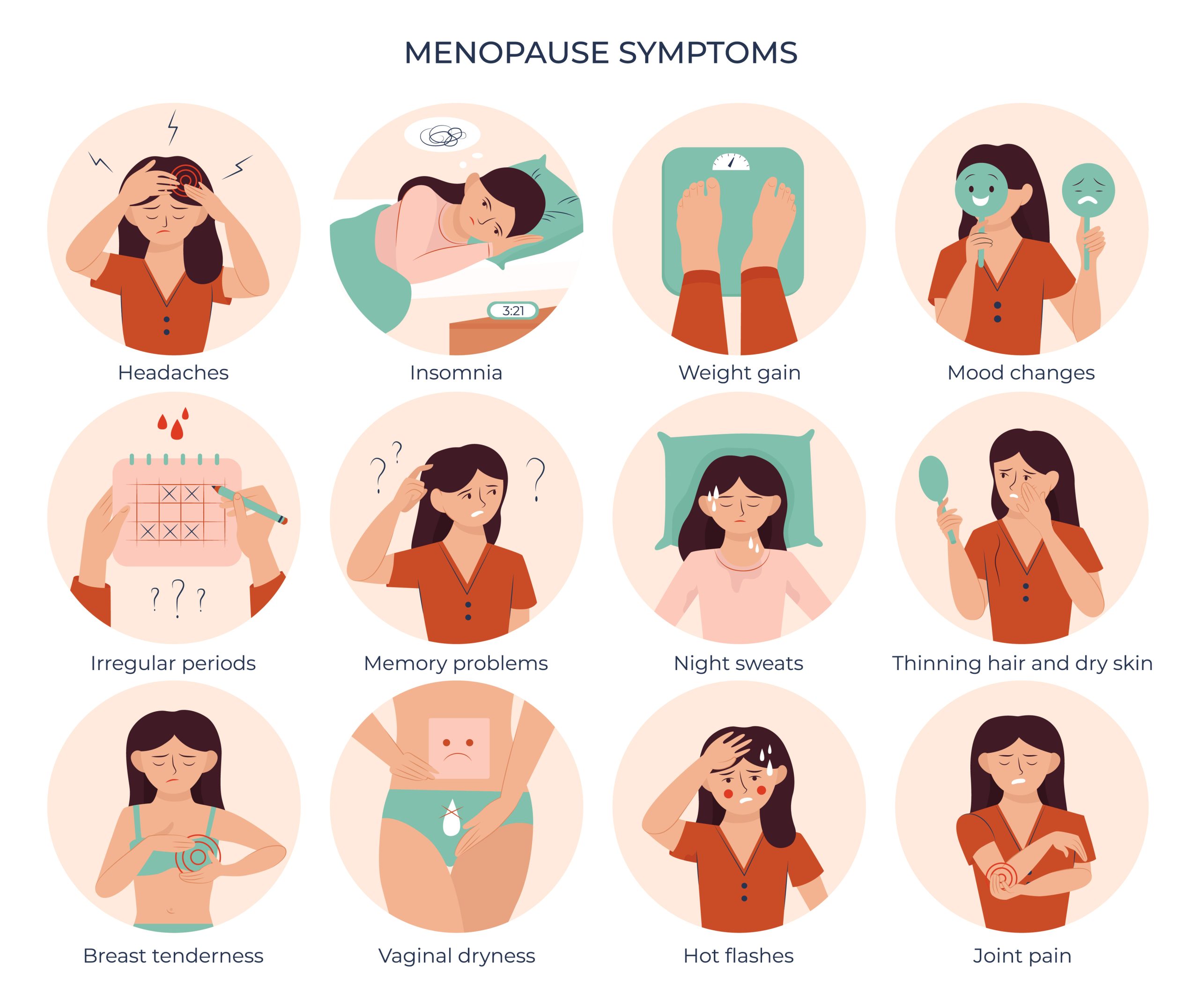
Over 80% of women experience symptoms during the menopause transition. Common issues include:
- Hot flushes and night sweats
- Irregular periods or changes in menstrual flow
- Weight gain, especially around the middle
- Mood swings, anxiety, low mood
- Poor sleep and fatigue
- Brain fog, forgetfulness, difficulty concentrating
- Joint pain, headaches, palpitations
- Vaginal dryness and reduced libido
- Digestive changes, bloating or constipation
- Hair thinning and dry skin
Symptoms can last for years and vary in intensity, with around 25% of women experiencing severe symptoms that affect daily life.
Why is Menopause Associated with Weight Gain?
Weight gain during menopause is common. On average, women gain 1.5 kg per year during menopause, adding up to 10 kg by the end of the transition. There are several reasons:
- Falling oestrogen levels affect where fat is stored, shifting it to the abdomen
- Lean muscle mass declines, reducing your resting metabolic rate
- The body becomes more insulin resistant, making it harder to process sugars
- Chronic low-grade inflammation increases water retention and fatigue
- Tiredness and low energy reduce physical activity levels
- Cravings and emotional eating become more common
It is not just about calories. The hormonal changes affect how your body stores and uses energy.
How can Weight Loss Medication Help?
GLP-1 medications, such as Wegovy or Mounjaro, can support women struggling with menopausal weight gain. These medications:
- Improve insulin resistance and help regulate blood sugar
- Delay stomach emptying, which helps you feel full for longer
- Reduce hunger and food cravings
- Support smaller portion sizes and better food choices
Used correctly, GLP-1s can be an effective tool. However, they are not a silver bullet. Lasting success comes from combining medication with the right nutrition, exercise and, where appropriate, hormone therapy.
Nutrition and Exercise Advice for Menopause

Your body’s needs change during menopause, so your approach to food and movement should evolve too.
Nutrition Advice
Focus on:
- Lean protein with every meal to support muscle mass (e.g. fish, chicken, tofu, eggs, pulses)
- Healthy fats to support hormone health (e.g. olive oil, nuts, avocado, oily fish)
- Fibre for digestion and energy balance (e.g. wholegrains, vegetables, legumes)
- Fermented foods for gut health (e.g. yoghurt, sauerkraut, kefir)
- Hydration – aim for 2 to 3 litres of water or herbal teas each day

Reduce:
- Processed foods and hidden sugars
- Excess caffeine and alcohol
- Portion sizes – reduce calorie intake by 300 to 500 calories per day
- Snacking, especially late at night
Try to eat three balanced meals per day, with mindful attention to hunger and fullness cues. Time-restricted eating, such as a 10-hour window (e.g. 8am to 6pm), may also support metabolism.
Exercise Advice
The goal is to maintain muscle mass, improve energy, and reduce long-term health risks.
Focus on:
- Resistance training (e.g. bodyweight exercises, dumbbells, resistance bands)
- At least two strength-based sessions per week, for 20 minutes or more
- Daily movement – walking, climbing stairs, swimming, cycling, or yoga
- Activities you enjoy and can stick with long term

Even small efforts add up. Just 2.5 hours of activity per week can reduce cardiovascular risk by 15%.
Thriving Through & Understanding Menopause
With the right support, weight gain during menopause is manageable – and even reversible. The most effective approach combines:
- Medical support – hormone therapy (HRT) or GLP-1s if appropriate
- Personalised nutrition – protein, fibre, and balanced portions
- Movement – resistance and aerobic training to preserve muscle and energy
- Mindset – building sustainable, long-term habits
This is not about going on a strict diet. It is about learning to fuel your changing body and supporting your long-term health, as well as giving you a better understanding of the menopause.
Impact of Weight Loss Medication on Progesterone Absorption
Weight loss medications such as GLP-1 receptor agonists (e.g. Wegovy or Mounjaro) can slow down how your digestive system works. This may reduce the absorption of oral medications, including progesterone.
If you are taking oral progesterone as part of your HRT or contraceptive, this reduced absorption may mean you are not getting the full dose your body needs. As a result, additional protection may be required:
- Consider switching to a Mirena coil, which delivers progesterone locally and is not affected by digestion
- Alternatively, your doctor may recommend temporarily increasing your oral progesterone dose
- This additional protection is especially important when you start GLP-1 medication or increase your dose
We strongly recommend speaking to your doctor to review your current HRT or contraceptive plan and ensure you remain fully protected throughout your treatment.
Next Steps
If you are already on a GLP-1 programme or considering it, speak to your CheqUp Health Coach about how your symptoms may relate to menopause and what support is available. You can also talk to your GP about hormone therapy options, or visit a menopause specialist clinic for personalised care.
We are pleased to recommend the Menoclinic, a specialist menopause partner who can help with 1:1 treatment solutions & give you a better understanding of the menopause.
You do not need to navigate this alone.


















